What is amblyopia?
Amblyopia, sometimes known as "lazy eye", is poor vision in an eye that did not develop normal sight during early childhood.
The best time to correct amblyopia is during infancy and early childhood or poor vision will be permanent. Parents must be aware of this potential problem if they wish to protect their child's vision.
Amblyopia usually only affects one eye, and is often due to poor focusing or a turned eye (a squint or strabismus). Rarely it may be due to cloudiness of the normally clear eye tissues.
It is common affecting 2-3 out of 100 people.
How is it detected?
It is not easy to recognise amblyopia. Young children with poor vision are unaware of the problem. Unless a child has a misaligned or turned eye, or other obvious abnormality, there is often no way for the parents to tell that something is wrong.
Amblyopia is detected through community vision screening and surveillance programs. Children with a family history of a turned eye, or a serious congenital eye condition such as a congenital cataract may be referred to be seen by a medical eye doctor (an Ophthalmologist).
How does normal vision develop?
Newborn infants are able to see, but as they use their eyes during the first months of life vision quickly improves. During early childhood the visual system continues to develop. By the age of 7-8 years, the visual system is fully developed and the nerve pathways cannot be changed.
The development of good vision in both eyes and straight eyes is necessary for normal vision. Some occupations are not open to people who have good vision in one eye only. If the vision in one eye should be lost later in life from an accident or eye disease, it is essential that the other eye has good vision.
When should vision be tested and who does it?
The Well Child-Tamariki Ora makes the following recommendations:
Plunket also undertakes pre-school vision testing.
Pre-school testing is not universally available through VHT in Auckland.
Free Pre-school testing is available in South Auckland through an independent Government funded Pre-school Vision Screening Programme. It is available for all children attending early childcare centres, and also available at other community venues.
How is amblyopia diagnosed?
Poor vision does not always mean that a child has amblyopia. Some focusing problems which may need glasses to correct, do not cause amblyopia.
The Ophthalmologist will use a variety of tests to measure vision. Drops will be used to dilate the child's pupils and temporarily stop their focusing in order that the need for glasses can be assessed. The inside of the eye will also be carefully examined to look for other causes of poor vision.
How is amblyopia treated?
Glasses may be prescribed to correct errors in focusing, and to help straighten a squinting eye. If glasses alone do not improve vision then eye patching is necessary. The better seeing eye is patched or covered for a period of time each day, often for weeks or months. Occasionally, amblyopia is treated by blurring the vision in the good eye with special drops to force the child to use the amblyopic eye. Part time patching treatment may need to occur until 8 years of age. After this age amblyopia usually does not return.
Does the treatment work?
Success mainly depends upon:
Is there financial help for purchasing the glasses?
There is a Government subsidy available to assist children from low-income families with vision problems (Community Service Card, High Health Use Card). The subsidy is available to children under 8 years of age.
The child is entitled to a maximum of $281.25 inc GST per year.
An Optometrist or Ophthalmologist determines entitlement.
Useful Contacts:
The Save Sight Society is affiliated with the Blind Foundation.
What is a cataract?
The lens of the human eye is similar to the lens of a camera. Located near the front of the eye, the lens focuses light on the retina at the back of the eye. Light passes through it to produce a sharp image on the retina. When the lens of the eye becomes cloudy or opaque, light is unable to pass through it and the vision is blurred. This condition is known as a cataract.
The cataract forms inside the eye and, contrary to popular misconception, is not a film which is visible on the surface of the eye.
How do they occur?
Cataract, the clouding of your lenses, are usually a natural part of aging. They can also exist at birth, be caused by an injury, or be caused by diseases like diabetes. Cataracts usually develop in both eyes, although not always at the same rate.
Cataracts are caused by an alteration of the protein structure within the lens of the eye as a person ages. The vast majority of people with cataracts are healthy and have no other eye disease.
By knowing how a normal eye works and how cataracts develop and affect your vision, you can better understand how cataracts are treated.
Eye with normal lens
In a normal eye the clear cornea allows light to enter. The coloured iris controls the amount of light entering the eye by changing the size of the pupil (opening). Light passes through a clear lens, which is surrounded and supported by a capsule, then through the vitreous (a clear gel that fills the eye). The light is focused by the lens onto the back of the eye, the retina, creating a sharp image. The image is then transmitted to the brain by the optic nerve.

Normal lens
Cataract lens
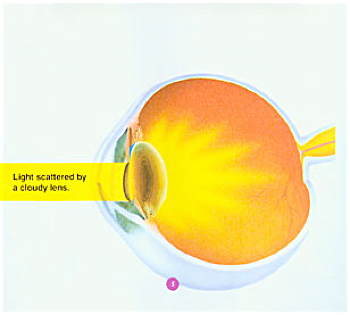
Eye with cataract
In an eye with a cataract, light passes through a cloudy lens. The lens scatters the light, causing blurring and glare. And because the cataract blocks light less of it is able to enter the eye, making it harder to see in dim light. A cataract on the edge of the lens may not affect the way you see. But a cataract in the middle of the lens may reduce your vision and is likely to interfere with your vision or perception of colour.
How do they affect you?
Cataracts often take a number of years to develop and may not cause problems in their early stages. Cataracts progress at varying rates from individual to individual. But as they develop they can reduce your sight and interfere with your lifestyle. You will notice a blurring of vision, sometimes with some "ghosting". Your eyes may become more sensitive to light and glare.
How are cataracts treated?
Because a cataract is a clouding of - not a film over - your lens, surgery is the only way to remove a cataract once it is formed. The operation involves making a small 1/3 of a centimetre opening into the eye, through which is put a small instrument which breaks the cataract up into small pieces so that it can be removed. This is called phacoemulsification. After that, a small clear plastic lens (the implant or IOL - introocular lens) is put into the eye to take the place of the cloudy lens (cataract) which has been removed. The whole operation takes around half to three quarters of an hour. Surgery is done on only one eye at a time. That way you can use the other eye while the eye that has been operated on heals.
Phacoemulsification

After a small incision is made in the eye, an extremely fine precision tip is inserted into the nucleus (main portion). High-frequency sound vibrations are used to break up the lens material, and the fragments are suctioned out. The posterior (back) capsule is left behind, reducing the risk of complications later on.
Posterior Chamber Lens Implant
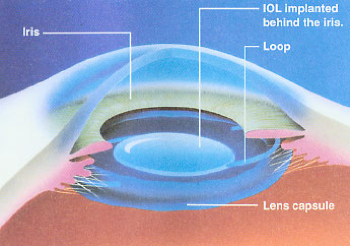
Unlike a contact lens that can be removed, the IOL becomes a permanent part of your eye. During the operation an IOL is placed in the posterior chamber (a space behind the iris) and held in place by flexible loops or tabs. The incision may be closed with stitches or with a no-stitch procedure.
Ultrasound Test
Prior to surgery the eye is measured in order to determine what strength your new implant lens will be. This is done by ultrasound waves. The test is painless and performed in the consulting room.
Anaesthesia - What type?
The operation can be done either under local or general anaesthetic. Under local anaesthetic, the anaesthetic is put on and around the eye. The majority of patients prefer this method. If, however, you are apprehensive about being awake during this operation, or have a problem such as an uncontrollable cough, twitch, etc, which would interfere with the operation, it is better for you to have a general anaesthetic. Your surgeon will discuss which is the preferred method for you.
Can cataracts be removed by laser?
Because a cataract is a clouding of lens, it cannot be removed with a laser. Occasionally, however, a very small amount of cataract can grow back some months after the operation, and this can be removed with a laser. This is a very short outpatient procedure.
Surgical pathway - what to expect
Day of surgery
Shortly after you are admitted to the hospital some eyedrops will be put in your eye to enlarge the pupil, making it easier to operate on the cataract.
Patients having a local anaesthetic need not lie rigidly still during the whole operation. The surgeon will tell you when it's important not to move. If you wish to move to make yourself comfortable please tell your doctor this.
After the operation
A pad may be placed over your eye which should be left in place until the following morning. You will need to come back to see your surgeon the following day. On bright days wear dark glasses. Put the eye drops, which you will be given, into the eye as instructed by the surgeon until they see you again. Pain relief tablets may be needed for a day or two.
You can resume normal activities. There is a misconception that after the operation you should not bend or stoop, cough, etc, but this is not the case. You may take a bath, shower, or wash your hair.
Immediately after the operation objects will look much brighter, but a little out of focus. In view of this you should not drive immediately after the operation. Your glasses will need to be changed, and this is normally done a few weeks after surgery.
Some patients see black spots (called floaters) in the vision. These are usually inconsequential, but inform your doctor when you next visit. You may also notice halos, glare and distortion of lights, particularly at night. You will also experience a little grittiness as the wound heals. All these symptoms recede with time.
After the operation it is most important to report to your surgeon if your eye becomes increasingly painful, or the vision progressively blurred.
Cataract surgery is usually successful with a greater than 95% chance of greatly improved vision. As with any operation, however, there is always some risk of complications, such as infection or haemorrhage. Fortunately, these occur rarely.
Cataracts don't have to interfere with the quality of your life. Your ophthalmologist can work with you to help improve your vision so you can return to the activities you enjoy.
If you can read, drive, watch the delight on a child's face, or gaze at a sunset …… Think how the gift of sight can make a real difference in someone's life. Eye donation is a precious gift given by a generous donor and their family.
The New Zealand National Eye Bank is a charitable non-profit organisation dedicated to the prevention of blindness by the provision of donated corneal and other tissues.
What is Diabetic Retinopathy?
Diabetes damages the blood vessels which supply the retina of the human eye. When signs of damage are detected, a person has "Retinopathy".

The Normal Retina
The retina is a very thin and complex layer which lines the back and inner wall of the eye, and contains the photoreceptors cells which convert light to chemical and electrical energy which is conveyed to the brain via other retinal cells, the optic nerve and the visual nerve pathways to produce, after much further processing, our sense of "vision" or seeing things in our environment. It is likened to the film of a camera. If the retina is damaged, especially in its central area (the Macula), there is irretrievable loss of sight.
The Macula with its central areas, the fovea and foveola, contain the "cone" photoreceptors responsible for colour and detailed vision (e.g. reading). Light is focused on the central macula by the lenses of the eye. The rest of the retina is principally "rod" photoreceptors which enable us to have some vision in low light levels. It is vital in treating diabetic retinopathy that the central macula area is preserved.
The inner half of the retina receives its blood supply from the central retinal artery which enters via the optic nerve. Diabetes causes the small blood vessels within the retina to close and/or leak blood, fats, and fluid, all of which are toxic to the retina which causes two types of major damage:

The Retina showing Diabetic Maculopathy
Proliferative Retinopathy
Closure of small blood vessels leads to proliferation of abnormal blood vessels which are fragile and may bleed into the vitreous (the "jelly" of the eye which fills the space between the retina and the lens) and may eventually cause the retina to detach.
Maculopathy
Leakage within the macula, especially of fluid and fat (exudates), destroys the retinal photoreceptor and "nerve" cells, and reduces "visual acuity" i.e. ability to see the vision test chart.
Retinopathy is graded according to severity and your Ophthalmologist (eye doctor) may tell you about these:
Laser Treatment
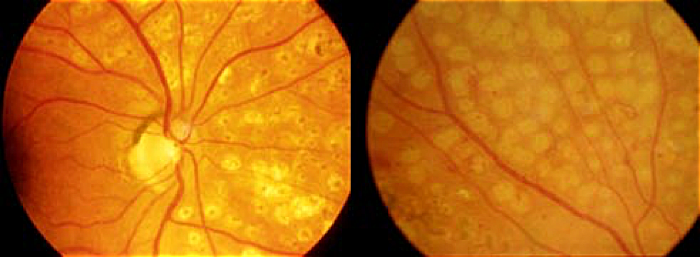
The Retina after Laser Treatment
This treatment is the only effective way of controlling sight-threatening retinopathy. It is most effective if able to be undertaken before retinopathy is advanced, and when vision is threatened by signs of impending vision loss rather than already reduced. Macula laser treatment "dries up" the fluid and exudates – but may take several months, and 2-3 treatments to be effective. Overall retinal laser treatment i.e. laser burns throughout the retina, causes the fragile abnormal blood vessels to disappear, or never develop. Again, several treatments may be necessary to each eye. Where treatment has to be extensive there will be some loss of side vision and night vision.
Retinopathy and Diabetes Type
Two main types of diabetes mellitus are recognized and retinopathy can occur in both:
People most likely to develop Retinopathy are those:
Preserving Vision in Diabetes
Regular Eye Examinations for Retinopathy
People with diabetes should all be referred by their Family Doctor for a routine retinal examination at least every 2 years because there is no other way of detecting retinopathy. This is done:
Benefits of regular eye examinations
Are eye checks necessary if diabetes is mild and diet controlled?
Yes. The risk is only slightly less in diet controlled diabetes.
Are eye checks necessary if diabetes control is very good?
The risk is considerably reduced, but other factors can influence retinopathy development.
Is fluctuating vision a sign of developing retinopathy?
Yes, it can be due to retinopathy or due to fluctuating (high) blood sugar affecting the lens of the eye. It may be due to the onset of Presbyopia (need to wear glasses for close work) which usually starts to occur from mid-forties onwards.
Is there any point in putting a big effort into diabetes control if a person with diabetes already has retinopathy?
Yes there is! There is strong evidence that progression of retinopathy can be slowed by about 50% in many patients with Mild or Moderate disease. However, retinopathy is not slowed by improved blood glucose control when it is advanced, but response to laser treatment may be better.
Pain from laser treatment – numerous concerns
Most people who have macula treatment do not experience pain. Treatment to the peripheral retina may cause transient pain and a dull ache for a few hours following treatment. The ophthalmologist will take measures to reduce pain from laser treatment.
Does laser treatment cause blindness?
In many people retinopathy is detected too late e.g. after a bleed into the vitreous from proliferative disease or with advanced fluid and lipid accumulation in the central macula causing much retinal damage and established vision loss. In such cases vision cannot be restored, but laser treatment is used to attempt to retain some sight. In some advanced proliferative cases, bleeding into the vitreous may occur and/or retinal detachment and this may be associated with laser treatment. However, such complications would have occurred without treatment and the eye is in a better state if some laser has been undertaken should surgery be necessary to remove blood from inside the eye and re-attach the retina.
How soon do the benefits of laser treatment become evident?
Laser is extremely effective in most patients treated, but benefits may not occur for some months after it is finished. Vision may improve for a long time as the retinopathy stablises.
After laser treatment is finished, will it need to be repeated each year or so?
This may be necessary in some persons with macular disease if the disease remains active and recurs in areas of the macula not previously requiring treatment. It is seldom necessary for proliferative disease once all the abnormal blood vessels have gone.
Can a patient tell if diabetes is affecting their eyes?
As indicated, occasionally fluctuating vision is a clue. However, in early retinopathy there are no symptoms, and visual acuity is normal (unless cataract or other disease affecting sight is present). Hence, the need for routine retinal examinations.
Further Information about Diabetes and Retinopathy:
What are the main causes of work-related eye injuries?
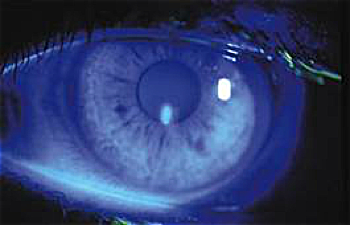
Corneal abrasion stained by fluorescein dye
Projectiles (for example, from abrasive blasting or grinding) or fixed or moving objects (for example, accidental stabbing of the eye from exposed sharp objects or tools) may strike the eye and cause a graze, contusion, tear, perforation or penetrating eye injury. Penetrating injuries are more likely to occur from missiles produced by striking metal-to-metal, for example, when hammering nails. Blunt trauma to the face around the eye can also cause lacerations to the eyelids causing poor eyelid closure with resultant eye surface damage from exposure, lacerations to the lacrimal (tear) drainage system and fractures around the eye that may lead to double vision, disfigurement and sometimes loss of vision.

Rusty corneal foreign body
Corrosive chemicals, hot liquids, irritant liquids, dust and gasses may cause severe corneal scarring leading to visual loss and disfigurement. Radiation from welding flash, industrial laser beams and infrared radiation can lead to visual impairment by causing burns to the retinal (nerve) layer inside the eye.
What can I do if someone had splashed corrosive chemicals or has irritant particles such as cement dust in the eye?

Blood in the anterior chamber of the eye (hyphaema) as a complication of blunt trauma. Eyes with hyphaema may show other signs of damage
IRRIGATE IMMEDIATELY!
Speed and time of irrigation is essential in preserving vision. The affected eye should be irrigated continuously for at least 15 minutes with clean cold water.
Do not attempt to remove contact lenses before or during continuous irrigation. The irrigation may wash the contact lens out or move it to be further back under the lids, the lens can be removed when medical attention is available. Refer to Emergency Department or Eye Casualty Service if available for further irrigation, removal of foreign body, assessment of damage and treatment.
What can I do if someone has had a blow to the eye?
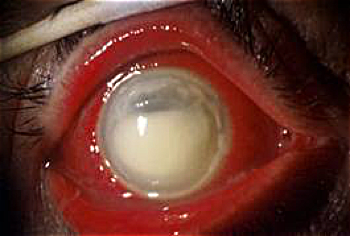
Severe alkali burn causing opacification of the cornea
If the injury is obviously major, prevent the patient from rubbing the eye or putting any pressure on the eye, especially if a penetrating eye injury is suspected. Cover the eye with a soft bandage (and eye shield if available) and go to hospital immediately. Do NOT attempt to remove any foreign body.
What can I do to protect my eye at work?
Further information:
Glaucoma is the number one preventable cause of blindness in New Zealand. Most of the time glaucoma is not associated with any pain or vision loss until the disease is very advanced. The only way for glaucoma to be diagnosed is by special tests done by an eye care professional, that is, an optometrist or ophthalmologist. Therefore, you should be tested for glaucoma as early detection and treatment will give you the best possibility of retaining your sight for your whole life.
Glaucoma New Zealand, an organisation which encourages early detection and treatment of this disease. Glaucoma New Zealand is linked to the Save Sight Society and the two groups work closely together to advance common objectives.
Age-related Macular Degeneration (AMD) is the leading cause of vision loss in the western world, and typically affects people over 60 years old.
What is the Macula?

The eye is like a camera. The cornea and the lens focus light onto the retina, which lines the back of the eye and acts like the photographic film in a camera. The macula is the central part of the retina and is responsible for our ability to see fine detail, for reading, driving and recognising faces. The Macula is also responsible for colour vision.
What is AMD?
With AMD there is damage or breakdown of the macula. Although AMD causes blurring of the central vision and thus impairs reading especially, it does not affect side vision so it does not result in total blindness. People with this complaint usually retain reasonable getting-about vision.

Normal eye
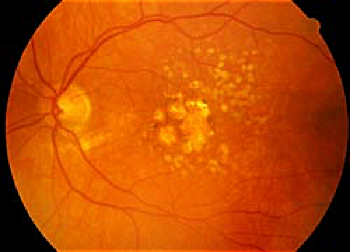
AMD
What are the Symptoms of AMD?
In its early stages there may be no significant effect on vision. Usually the first symptoms are loss of clarity when reading. As the complaint progresses the ability to watch television and to drive safely will be impaired. Sometimes AMD affects one eye more than the other and so people can often cope for quite a while before it becomes disabling.
Can AMD be prevented?
The exact cause of this complaint is unknown but a healthy life style without smoking and having a good diet will reduce the risk of it occurring.
Can AMD be treated?
There is no treatment for Dry ARMD, although high dose multivitamin combination has been shown to decrease the risk of visual loss from ARMD over 5 years in high risk patients.
There are a few treatment options for Wet ARMD although the best outcomes occur when this disease is detected early. These are thermal laser, Photodynamic Therapy, newer injections to new blood vessel growth called anti-VEGFs, or combinations of these. Not all patients will be candidates for these treatments, and treatment may not prevent further vision loss.
How will I know I have ARMD?
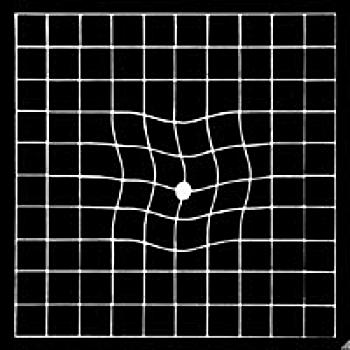
Early reporting of new distortion or blurriness should be reported and referred to an ophthalmologist. The earlier the disease is detected, the more likely it will be amenable to treatment, and the loss of vision will be lessened. The earliest inkling is distortion of straight lines, making a grid pattern appear like this:
It is important to consult with an eye specialist if this should occur because laser treatment can sometimes slow down the rate of loss of vision.
Can Glasses improve the vision?
Stronger glasses only have a limited ability to improve the vision in this complaint. Often those suffering from advanced AMD require special magnifying devices, which are either available from Optometrists or special low visual aid clinics which are often attached to the Eye Department in larger hospitals.
What else can be done?
It is important to have good lighting, preferably a reflector reading lamp, when doing close work.
Continue doing as much reading as you can, you cannot "save your eyes" by avoiding reading, sewing etc. There is a wide range of support services available to help those with AMD. The Royal New Zealand Foundation for the Blind gives helpful advice.
It is important to emphasise however that those with this complaint never become totally blind.
Further reading
"The challenge of Macular Degeneration" by Hui Sun and Jeremy Nathans
Scientific American October 2001 page 60
For more information:
The Save Sight Society is affiliated with Retina New Zealand.
|
|
Further InformationFor more information please fill out our contact form. |